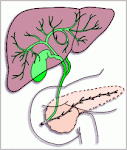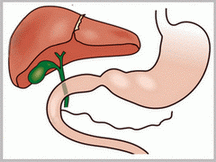
Gallbladder symptoms
Table of Contents
About me
Categories
Text
Gallbladder Symptoms
By David Moriss
How to recognize and treat gallbladder symptoms
When a vital organ is declining in health it's going to tell you subtly at first, then more strongly and finally it will scream at you until you get the message. Gallbladder symptoms work in this way as well. You may start with some pesky constipation, then perhaps you notice that you're bloated and bilious after most meals, after that you start to feel pain under the right side of your rib cage, and the next thing you know the pain is radiating through your back and shoulders and you feel absolutely sick and dizzy.
This is the general progression that gallbladder symptoms will take. Beginning with the more subtle signs and ending with the severe signs, it truly is like your body is gently nudging you at first saying, "Excuse me.....but there's a problem down here," and when you continuously ignore these signals, or write them off as being "normal", then your body must resort to hollering "There is a SERIOUS problem going on!!!" When you ignore the signs and symptoms of your gallbladder, you'll end up with gallstones and disease-it's that simple.
Millions of Americans are afflicted with gallbladder disease, and the majority of them don't listen to the symptoms until they're suffering a full attack. At that point, they'll generally go to their doctor who will tell them it's smart to completely remove the gallbladder. Gone....finito.....no more! Once they remove that gallbladder-- because they had ignored its signals for so long-- they can never get it back and they're forced to deal with seriously compromised digestion for the rest of their lives, not to mention exorbitant medical bills, painful recovery, and the loss of an organ that could have been revived naturally......
You heard me right-the gallbladder can be naturally revitalized once you listen to the alarm bells and act in accordance. Because most folks respond to the signs when it's too late, they don't realize that they can capitalize on a natural, simple, inexpensive, and healing cleanse that can not just cure their gallbladder and gallstones but can also renew their entire health in a way that they never conceived as possible! There have been 1000s of folks across the nation who have discovered the secret to gallbladder wellness and you can be one of them as well. All you have to do is act now. Don't wait until the inevitable happens. You can keep your gallbladder and be healthy at the same time.
For more information on gallbladder symptoms and gallbladder cleanse, visit the links.
Article Source: http://EzineArticles.com/?expert=David_Moriss |
Labels: Gallbladder symptoms
Abdominal pain is one of the commonest symptoms that gastroenterologists encounter both in outpatients and inpatients. This can sometimes provide a major diagnostic challenge, particularly in patients who are unable to give a good history. However, a good history, thorough examination and a basic understanding of typical patterns and clinical presentations of common diseases should help in making a diagnosis in most cases.
Abdominal pain can be categorized as visceral, parietal or referred. Visceral pain is dull and aching in character. It is poorly localized and is usually secondary to distention or spasm of a hollow viscus. Parietal pain is sharp and well localized and arises from irritation of the parietal peritoneum. Referred pain is the perception of pain at a site distant from the origin of the stimulus. One possible explanation for this is that the visceral and the somatic afferent nerve fibers share a common pathway at the level of the cord, which is the spinothalamic tract. The brain tends to associate the stimulation more with a somatic source rather than visceral. This type of pain is characteristically aching and perceived to be near the surface of the body. For example, referred pain from gallstones is sometimes perceived in the right shoulder because some of the afferent pain fibers run in the right phrenic nerve (C3–5).
It is important to have a basic understanding of some of the physiological factors that cause abdominal pain. The main visceral pain receptors in the abdomen respond to mechanical and chemical stimuli. The mechanical stimuli perceived are stretch, distention, contraction, compression and torsion. The chemical stimuli include substance P, bradykinin, serotonin, and prostaglandins. These receptors are located on the serosal surfaces, within the mesentery and within the walls of the hollow viscera.
Gut-related visceral pain is usually perceived in the midline because of bilateral symmetric innervation, except for pains originating from the gallbladder and the ascending and descending colon. Pain originating from other intra-abdominal organs generally tends to be unilateral.
The perception of visceral pain corresponds to the spinal segments where the visceral afferent nerve fibers enter the spinal cord. For instance, distention of gallbladder causes discomfort in the Epigastrium (T7–T9).
Labels: Gallbladder symptoms
Gallstones may be present for decades before symptoms develop, and 70% to 80% of patients remain asymptomatic throughout their lives. It appears that asymptomatic patients convert to symptomatic ones at the rate of 1% to 3% per year, and the risk diminishes with time. Prominent among symptoms is biliary pain, which tends to be constant, or an excruciating "colicky" (spasmodic) pain due to the obstructive nature of gallstones in the gallbladder or biliary tree proper. Inflammation of the gallbladder, in association with stones, also generates pain. More severe complications include empyema, perforation, fistulas, inflammation of the biliary tree (cholangitis), and obstructive cholestasis or pancreatitis with ensuant problems. The larger the stones, the less likely they are to enter the cystic or common ducts to produce obstruction--it is the very small stones, or "gravel," that are the more dangerous. A large stone may occasionally erode directly into an adjacent loop of small bowel, generating intestinal obstruction ("gallstone ileus"). On occasion, progressive mucosal removal of luminal lipids in obstructed, uninflamed gallbladders may leave clear mucinous secretions, so-called hydrops or mucocele of the gallbladder. Most notable is the increased risk for carcinoma of the gallbladder.
Patients with acute calculous cholecystitis usually but not always have experienced previous episodes of biliary pain. Acute calculous cholecystitis may appear with remarkable suddenness and constitute an acute surgical emergency, or it may present with mild symptoms that resolve without medical intervention. An attack of acute cholecystitis begins with progressive right upper quadrant or epigastric pain, frequently associated with mild fever, anorexia, tachycardia, diaphoresis, and nausea and vomiting. The upper abdomen is tender, but a distended tender gallbladder is not usually evident. Most patients are free of jaundice; the presence of hyperbilirubinemia suggests obstruction of the common bile duct. Mild to moderate leukocytosis may be accompanied by mild elevations in serum alkaline phosphatase values. In the absence of medical attention, the attack usually subsides in 7 to 10 days and frequently within 24 hours. However, up to 25% of patients develop progressively more severe symptoms, requiring immediate surgical intervention. In those patients who recover, recurrence is common.
Clinical symptoms of acute acalculous cholecystitis tend to be more insidious, since symptoms are obscured by the underlying conditions precipitating the attacks. A higher proportion of patients have no symptoms referable to the gallbladder; diagnosis therefore rests on a high index of suspicion. In the severely ill patient, early recognition of this condition is crucial, since failure to do so almost ensures a fatal outcome. A more indolent form of acute acalculous cholecystitis may occur in the outpatient population in the setting of systemic vasculitis, severe atherosclerotic ischemic disease in the elderly, and acquired immunodeficiency syndrome (with infection).
Chronic cholecystitis does not have the striking manifestations of the acute forms and is usually characterized by recurrent attacks of either steady or colicky epigastric or right upper quadrant pain. Nausea, vomiting, and intolerance for fatty foods are frequent accompaniments.
Labels: Gallbladder symptoms
Gallbladder Function
The gallbladder concentrates and stores bile secreted by the liver during the fasting state and delivers bile into the duodenum in response to a meal. Since the usual capacity of the gallbladder as a reservoir is only about 30 to 60 mL, the remarkable absorptive capacity of the gallbladder accounts for its ability to store much of the 600 mL of bile produced each day. The gallbladder mucosa has the greatest absorptive capacity per unit area of any structure in the body. Bile is usually concentrated 5- to 10-fold by the absorption of water and electrolytes leading to a marked change in bile composition.
Active sodium chloride transport by the gallbladder epithelium is the driving force for the concentration of bile. Water is passively absorbed in response to the osmotic force generated by solute absorption. The concentration of bile may affect the solubility of two important components of gallstones: calcium and cholesterol. Although the gallbladder mucosa absorbs calcium, this process is not nearly as efficient as for sodium or water, leading to greater relative increase in calcium concentration. As the gallbladder bile becomes concentrated, several changes occur in the functional capacity of the cholesterol solubility system . The solubility in the micellar fraction is increased, but the stability of phospholipid-cholesterol vesicles is greatly decreased. Because cholesterol crystal precipitation occurs preferentially by vesicular rather than micellar mechanisms, the net effect of concentrating bile is an increased tendency for cholesterol nucleation.
The gallbladder lining cell secretes at least two important products into the gallbladder lumen: glycoproteins and hydrogen ions. Secretion of mucus glycoprotein occurs primarily from the glands of the gallbladder neck and cystic duct. The resultant mucin gel is believed to constitute an important part of the unstirred layer (diffusion-resistant barrier) that separates the gallbladder cell membrane from the luminal bile. This mucus barrier may be very important in protecting the gallbladder epithelium from the strong detergent effect of the highly concentrated bile salts found in the gallbladder. However, considerable evidence also suggests that mucin glycoproteins play a role as a pronucleating agent for cholesterol crystallization. The transport of hydrogen ions by the gallbladder epithelium leads to a decrease in gallbladder bile pH through a sodium-exchange mechanism. Acidification of bile promotes calcium solubility, thereby preventing its precipitation as calcium salts. The gallbladder's normal acidification process lowers the pH of entering hepatic bile from 7.5 to 7.8 down to 7.1 to 7.3.
The gallbladder fills from the continuous production of bile by the liver against the force of a contracted sphincter of Oddi. As the pressure within the common bile duct exceeds that within the gallbladder lumen, bile enters the gallbladder by retrograde flow through the cystic duct, wherein it is rapidly concentrated. Periods of filling are punctuated by brief episodes of partial emptying (∼10%-15% of its volume) of concentrated gallbladder bile that are coordinated through the duodenum of phase III of the migrating myoelectric complex (MMC).
Following a meal, the gallbladder contracts in response to both a vagally mediated cephalic phase of activity and the release of cholecystokinin (CCK), the major regulatory hormone of gallbladder function. In the next 60 to 120 minutes, about 50% to 70% of gallbladder bile is steadily emptied into the intestinal tract. CCK is localized to the proximal small intestine, especially the duodenal epithelial cells, where its release is stimulated by intraluminal fat, amino acids, and gastric acid and inhibited by bile. In addition to stimulating gallbladder contractions, CCK also acts to functionally inhibit the normal phasic motor activity of the sphincter of Oddi. Gallbladder refilling then occurs gradually over the next 60 to 90 minutes.
Labels: gallbladder
GALLSTONES
Gallstones are extremely common and will affect one in three women and one in five men. Most stones are totally asymptomatic and are found by chance during other investigations. There are three types of gallstones.
* Cholesterol stones are often solitary; they form in bile in which cholesterol is in excess relative to bile salts, and are
found in about 10% of patients with stones; they are common in women who have had many children or who have taken oral contraceptives.
* Pigment stones are usually multiple and green—black in color; they account for about 10-15% of all stones and are the result of bilirubin precipitation, caused by overproduction in chronic haemolytic states; they are later associated with recurrent ascending cholangitis.
* Mixed stones are by far the most common, are usually multiple and are a mixture of cholesterol, pigment, calcium carbonate and phosphate; they are found in people who are obese, who have taken estrogen or who have lived on a diet rich in unrefined carbohydrate and high in calories.
In most patients stones form and remain in the gallbladder without causing symptoms, but they may produce a range of symptoms, including intolerance to fatty foods, with nausea, vomiting, flatulence and epigastric pain. In a minority of patients, gallstones may be associated with significant complications.
Migration of stones may lead to additional symptoms such as colicky right hypochondrial pain, obstructive jaundice and recurrent bouts of ascending cholangitis or acute pancreatitis, or both.
Chronic cholecystitis may lead to adhesion of the gallbladder to surrounding organs, for example the small bowel, colon or
stomach, with subsequent erosion of a stone, which may then pass along the bowel and even cause intestinal obstruction if very
large. The presence of a fistula leads to recurrent ascending infections in the biliary tree. Chronic cholecystitis may lead to carcinoma of the gallbladder.
The principal mode of therapy is surgery. Gallstones may be removed by a course of extracorporeal shock-wave lithotripsy in association with oral bile acid (ursodeoxycholic acid) dissolution therapy. This is a lengthy and tedious procedure which has a 30-80% success rate after 1 year.
What are the complications of gallstone disease?
* acute cholestasis
* chronic cholecystitis
* fistula formation — gallstone ileus
* impaction of stone in common hepatic duct
* gangrene of gallbladder, perforation or empyema
* pancreatitis
Labels: Gallstones
What is Biliary colic?
Biliary colic is the most common symptom of patients with gallstones. Repeated low-grade inflammation can lead to chronic cholecystitis (a histological diagnosis), characterized by a thickened, shrunken and fibrosed gallbladder.
How common is biliary colic?
Biliary colic is common. The incidence is 2000 per 100 000 per year in patients with gallstones. The incidence decreases with time, to approximately half after 5 years as 30% of patients only ever experience one episode. The exact prevalence of biliary colic is difficult to determine as both gallstones and upper abdominal pain are common and often go undiagnosed.
Pathology
The symptoms of biliary colic arise from distension and spasm of the gallbladder from an impacted gallstone in the gallbladder neck obstructing the cystic duct and normal flow of bile. Once the impacted stone falls back from the gallbladder neck, the gallbladder empties and the pain ceases.
Scope of disease
Continued impaction of the stone results in chemical inflammation and can lead to acute cholecystitis. Recurrent episodes of biliary colic result in low-grade inflammation leading to chronic cholecystitis. Gallstone impaction in Hartmann's pouch when the gallbladder is empty may result in mucus secretion from the gallbladder leading to a mucocele.
Clinical features
Biliary colic is a misnomer, as the pain is typically constant. It is usually a severe pain experienced in the right upper quadrant or epigastrium. The onset of pain is rapid and the duration is usually more than 15 minutes, resolving within 24 hours. Biliary colic may be precipitated by fatty food and radiate to the scapula.
Examination reveals right upper quadrant tenderness in an afebrile patient. Fever, jaundice, Murphy's sign, systemic upset or signs of peritoneal irritation indicate the development of other complications. A palpable gallbladder suggests a mucocele.
Initial investigations
Full blood count, liver profile and amylase
Full blood count, liver profile and serum amylase are normal in biliary colic.
Ultrasound of the abdomen
Ultrasound scanning confirms the presence of gallstones in the gallbladder.
Further investigations
Upper gastrointestinal endoscopy
If ultrasonography is normal, upper gastrointestinal endoscopy should be performed to exclude peptic ulcer disease, gastritis and gastro-oesophageal reflux disease.
Initial management
Analgesia
Biliary colic is usually managed in the community with oral analgesics, but intramuscular diclofenac may prevent progression to acute cholecystitis. If analgesia is inadequate, hospital admission for intravenous opiates is required until the pain settles.
Surgical management
Cholecystectomy
Elective cholecystectomy has become the standard therapy for gallstones causing biliary colic. The advantages over medical therapy are: no restrictions on the number, size or type of gallstone, rapid stone removal, prevention of recurrence and elimination of any risk of gallbladder cancer.
Cholecystectomy may be undertaken with a laparoscopic or open approach Over the last decade, laparoscopic cholecystectomy has become the operation of choice by surgeons and the general public, such that the open approach is now seldom performed as the first choice. This is despite randomized trials showing similar outcomes when a small incision open approach is compared to the laparoscopic approach.
Labels: Gallbladder symptoms
Gallstones represent a failure to maintain certain biliary solutes, primarily cholesterol. and calcium salts in a solubilized state. Gallstones are classified by their cholesterol content as either cholesterol or pigment stones. Pigment stones are further classified as either black or brown. Pure cholesterol gallstones are uncommon (10%) with most cholesterol stones containing calcium salts in their center, or nidus. In most American populations, 70% to 80% of gallstones are cholesterol, and black pigment stones account for most of the remaining 20% to 30%.
An important biliary precipitate in gallstone pathogenesis is biliary sludge which refers to a mixture of cholesterol crystals, calcium bilirubinate granules, and a mucin gel matrix. Biliary sludge has been observed clinically in prolonged fasting states or with the use of long-term total parenteral nutrition (TPN). Both of these conditions are also associated with gallstone formation. The finding of macromolecular complexes of mucin and bilirubin, similar to biliary sludge in the central core of most cholesterol gallstones, suggests that sludge may serve as the nidus for gallstone growth.
Most gallstones form in the gallbladder (cholecystolithiasis). Gallstones found in the bile ducts (choledocholithiasis) commonly originate from the gallbladder but may develop within the ducts if biliary stasis is present. Some small gallstones (less than 5 mm diameter) probably pass unnoticed into the duodenum but larger stones may impact in the duct or ampulla of Vater, causing pain, obstructive jaundice, acute pancreatitis or acute cholangitis. Stones may also impact in Hartmann's pouch, and the secondary inflammation can obstruct the normal flow of bile into the common bile duct (Mirizzi's syndrome). The development of a fistula between the gallbladder and the duodenum can allow the passage of large gallstones leading to intestinal obstruction (gallstone ileus).
Labels: Gallstones